Why referral is its own skill
Recognising a sick child (which is the signs of acute illness in children chapter) is half the job. The other half is doing something useful with that recognition: getting the child into the hands of someone who can provide more than the educator can. That sounds simple — call the parent, call the doctor, call the ambulance — but in practice the right call to the right person at the right time, with the right information, is a skill that benefits from being thought through in advance. G10.1
This chapter is about that skill. It covers the pathways available to the educator, the criteria for choosing among them, the conversation with each (parent, GP, ambulance dispatcher, paramedic on arrival), the handover information they need, and the documentation that follows. The companion chapters in this topic are about the recognition that gets you here and about the action plans, communication, and physiology that fill in the surrounding picture.
§ Instructor's note
The teaching point of this chapter is the structure of the referral pathway and the discipline of a clean handover. Educators sometimes treat "call the parent" as the entire response when the child needs more — and conversely, they sometimes call 000 reflexively for situations the parent can manage with a doctor's appointment. The right answer is in the middle, and it depends on the urgency. Drill the rule: match the response to the urgency, give a clear handover, and stay with the child until someone else is in charge.
The pathways available
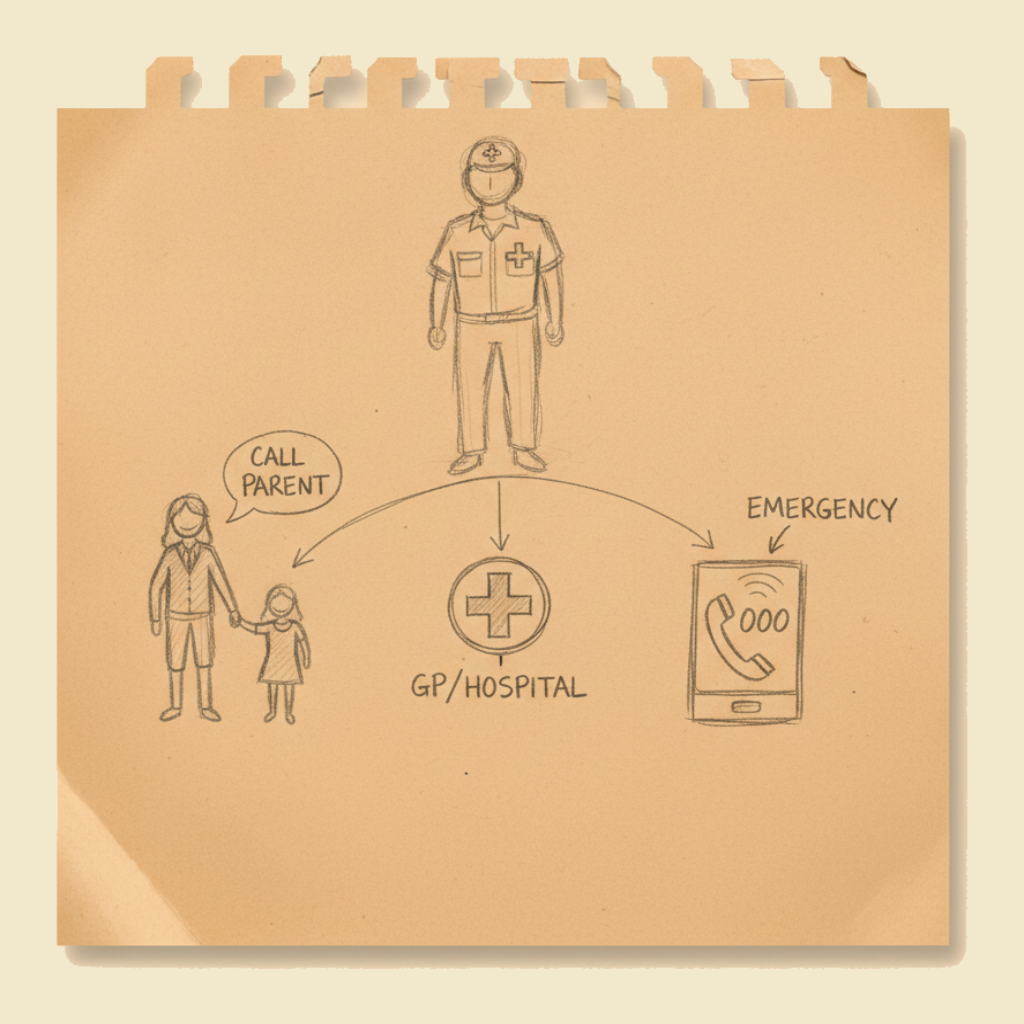
When the educator decides a child needs more than service-level care, the available pathways are:
- Parent collection and home care — for a child who is unwell but not seriously so. Most "send-home" cases.
- Parent collection and direct visit to the GP — for a child who needs medical assessment but is not in immediate danger. The parent makes the appointment or attends a walk-in clinic.
- Parent collection and direct visit to a hospital emergency department — for a child who needs more than a GP can provide but is well enough to be transported privately by the parent.
- Ambulance to hospital — for a child whose condition is serious enough that the educator should not wait for the parent to arrive before transport begins, or that warrants the level of care that paramedics can provide en route.
- 000 call with paramedic decision — when the educator is unsure of the urgency and wants the dispatcher to make the call about the level of response.
The decision tree, in approximate order of urgency:
- Life-threatening emergency (cardiac arrest, severe anaphylaxis, severe respiratory distress, status epilepticus, severe bleeding, severe head injury, drowning, severe burn, suspected meningococcal disease) → Call 000 immediately, then notify the parent. The ambulance will arrive and take over.
- Serious illness or injury that needs hospital but is not immediately life-threatening (suspected fracture with deformity, significant burn, suspected appendicitis, severe asthma not responding to puffer, moderate dehydration with deteriorating signs) → Call 000 or call the parent depending on the situation. If the parent can collect quickly and the situation is stable, parent transport may be appropriate. If not, the ambulance is the right answer.
- Moderate illness needing same-day medical assessment (high fever in a young infant, persistent vomiting, suspicion of an underlying condition, significant unexplained pain) → Call the parent with a clear recommendation that the child be seen by a doctor today.
- Mild illness needing rest at home (low-grade fever in an otherwise well child, single vomit episode, minor injury, viral cold) → Call the parent for collection in line with the service's exclusion policy. Medical assessment is the parent's choice.
The educator does not always have to make the choice alone. The nominated supervisor can advise, and the 000 dispatcher is trained to help with the decision when you call. There is no penalty for calling 000 and having the dispatcher tell you the situation does not need an ambulance. There is a real penalty for waiting too long to call.
Calling the parent
The first call in most situations is the parent. Even when 000 is the right call for the medical situation, the parent should also be contacted as soon as possible. The conversation has a structure:
- Identify yourself and the child — "Hi, this is Jess from Bright Stars. I'm calling about Mia."
- State the situation calmly and clearly — "Mia has just had a vomit and a runny nappy, and she's looking quite tired. She's resting in the quiet room with me."
- Give the relevant observations — what you have seen, when it started, what you have done, how the child is now.
- Make a clear request — "We'd like you to come and collect her, and I think she should be seen by a doctor today."
- Confirm the action and the timing — "OK, you can be here in 20 minutes. We'll have her ready for you."
- Give any instructions for what they should bring — change of clothes, comfort item, the child's medication.
- Reassure — "She's settled and comfortable, we'll keep an eye on her until you arrive."
- Offer the next contact point — "Call me back if you can't make it in 20 minutes, or if anything changes on your end."
If the situation is more urgent, the conversation is shorter and more direct: "Sam has had an asthma attack, we've given his puffer, the ambulance is on the way, and we need you to come straight here or meet us at the hospital."
For the most urgent situations, the order may be inverted — call 000 first, then call the parent — because the ambulance call is more time-critical and the parent's role is to follow the child rather than to make a treatment decision.
When the parent cannot be reached
The educator's response when the parent does not pick up:
- Try the secondary emergency contact on the enrolment form. Most services require at least one alternative contact for exactly this situation.
- Try the parent's workplace if the number is on file.
- Keep trying the primary contact in parallel.
- Continue the appropriate first aid while the calls are being made.
- If the situation is serious and the parents cannot be reached, do not let the search for parental contact delay urgent medical care. Call 000 if the child needs an ambulance regardless of whether you have reached a parent.
- Document every attempt with time, number called, and outcome.
- The nominated supervisor can take over the parent search while you focus on the child.
The parent's right to be informed does not override the child's right to receive timely care. See the parental consent chapter for the legal foundation.
Calling 000 — the conversation

Calling 000 is the educator's escalation to the highest level of immediate care. The conversation has a structure that the dispatcher will guide you through, but knowing the structure in advance helps you be useful rather than panicked.
When you dial 000, you are first asked which emergency service you need: police, fire, or ambulance. For a sick child, the answer is ambulance. You are connected to the ambulance dispatcher, who will then ask:
- The location — the address of the service. Be precise. If the service is in a complex with multiple buildings, include the building name and any access information. The dispatcher needs to be able to direct the ambulance to the right entrance.
- The phone number you are calling from — in case the call is dropped.
- The nature of the emergency — what is happening to the casualty.
- The casualty's age and sex — and any other identifying information.
- The casualty's condition — conscious or not, breathing or not, the symptoms you are seeing, the response to any first aid you have given.
- What has happened or is happening — the story of the incident.
- The first aid in progress — what you are doing now (CPR, EpiPen, oxygen, etc.).
The dispatcher may give instructions — start CPR, give the puffer, position the casualty, prepare for the paramedics' arrival — and may stay on the line until the ambulance arrives. Do not hang up until the dispatcher tells you to. The line is part of the chain of care and may include life-saving instructions.
Have someone (another educator) ready to:
- Open the gate or door for the ambulance.
- Direct the paramedics to the casualty when they arrive.
- Move other children away from the area where the paramedics will work.
- Find any medications, action plans, and the child's enrolment file to give to the paramedics.
- Continue trying to contact the parents.
This is a multi-person job and an educator working alone will struggle. Calling for help is the first action — another educator, the nominated supervisor, anyone in the service who can assist.
See the accessing emergency services chapter for more on the call itself.
Two common reasons for delayed 000 calls in education and care services: the educator is not sure of the precise address (particularly in a large complex or multi-building service), and the educator is not sure if the child is "really sick enough" to call. Both are removable. The address should be on a sticker next to every phone in the service — find out where, write it on a card, and stick it up. The diagnosis is not the educator's responsibility — the dispatcher will help, the paramedics will assess, and the worst that can happen if you call 000 unnecessarily is a brief check by the paramedics. The worst that can happen if you don't call when you should is much worse.
The handover to the ambulance
When the paramedics arrive, the educator who has been managing the child gives a handover — a structured summary that lets the paramedics take over the care without losing information. A useful structure is the ATMIST format used by ambulance services worldwide:
- A — Age — "This is Lily, she's 4 years old."
- T — Time of incident — "She had her first vomit at 10.15, about 45 minutes ago."
- M — Mechanism — "She'd been a bit off-colour all morning, then suddenly vomited at morning tea."
- I — Injuries / illness — "Vomiting, abdominal pain, lethargy, fever of 39.2."
- S — Signs — "She's tachycardic, pale, capillary refill 3 seconds, has been drowsy for the last 10 minutes, refusing fluids."
- T — Treatment given — "We've kept her in the recovery position, offered sips of water which she didn't take, called her mum who's on the way, and called you."
This is a 30-second handover that gives the paramedics everything they need to take over. They will ask questions to fill in the gaps, but the structured opening lets them think while you talk rather than having to drag information out of you.
Other things to give the paramedics:
- The child's enrolment file with medical information, allergies, current medications, and any action plans.
- Any medications the child has at the service (EpiPen, puffer, etc.) — the paramedics may want to take these with the child or they may want to know what has been given.
- The parents' contact details if they are not yet at the service.
- The educator's name and the service's name, in case the paramedics or hospital need to follow up.
- A clean account of what happened, in writing if there is time, for the medical record.
The paramedics will want to see the child immediately — do not delay the handover for paperwork. Give the verbal handover as they assess the child, then provide the written information once they are working.
Calling the GP or the hospital directly
Some situations are not 000-urgent but need same-day medical attention. In these cases the educator's role is to advise the parent to take the child to the GP or to the hospital emergency department, rather than to call directly. The reasoning:
- The GP or hospital does not have a relationship with the service the way the parent does.
- The medical assessment requires the parent's presence and consent.
- The parent is the legal decision-maker for non-emergency care.
- The GP or hospital cannot dispatch transport the way the ambulance can.
In some specific situations the educator may speak directly to a medical service — for example, calling the hospital where a child has been transported earlier in the day to update them on a development, or calling the child's specialist to follow up on a known condition. These are usually orchestrated through the nominated supervisor and the parent rather than initiated independently by the front-line educator.
The exception is when the educator has called 000 and the paramedics are arranging transport — in that case the paramedics liaise with the receiving hospital, and the educator's job is to provide the information needed for the handover.
After the ambulance has gone
Once the paramedics have taken over and the child has left the service:
- Stay with any other children affected by the incident — they may have seen things that frightened them. Reassure, provide a calm space, allow questions. See the rescuer and child stress support chapter.
- Brief the rest of the staff about what happened so they can answer questions from parents at pickup.
- Complete the documentation — the incident, injury, trauma and illness record, the description of the response, the timeline, the outcome.
- Notify the Regulatory Authority through the nominated supervisor if the incident meets the criteria for a notifiable incident under the Education and Care Services National Law. See the education and care services national law chapter.
- Follow up with the family later in the day — a phone call to find out how the child is doing is usually appreciated and is good practice.
- Debrief the staff who were involved in the response. See the rescuer and child stress support chapter again.
- Communicate with the wider parent community if the incident warrants it, in line with the service's communication policy and respecting the privacy of the child's family.
- Review the response in due course — what went well, what could be improved, whether any policies or procedures need updating.
The educator's job does not end when the ambulance leaves. The aftermath is part of the response.
When the situation is borderline
A common difficulty: the child is unwell but not clearly serious enough for 000, and the parent cannot collect immediately. The educator is left waiting, monitoring, and uncertain.
The right approach in these situations:
- Continue to assess the child every 5 to 10 minutes. Watch for any deterioration.
- Document each assessment with the time and the findings. The trend across the assessments is the most important information.
- Lower your threshold for calling 000 if the trend is worsening. A child who was borderline 30 minutes ago and is now worse is no longer borderline.
- Stay in contact with the parent with updates. They need to know if the situation is changing.
- Do not be afraid to upgrade to an ambulance call if the wait for the parent is too long for the child's condition. The parent can meet the ambulance at the hospital.
- Use the nominated supervisor as a sounding board for borderline decisions.
- Trust your instinct. If you are increasingly worried, that is itself information — escalate.
The biggest mistake in borderline situations is inertia — continuing to wait for the parent because that is the plan, even though the child is getting worse. The plan should be revised when the situation changes. The educator's job is to act on the new situation, not the old one.
Most services have a written escalation policy that maps observed signs to the response — when to call the parent, when to call the nominated supervisor, when to call 000. The policy is the operational version of this chapter and should be followed in preference to any general advice. Read it now, before you need it. If your service does not have one, raise it with the nominated supervisor — it is a useful piece of operational guidance and most services have one as part of their National Quality Standard documentation under Quality Area 2.
Preparing for ambulance access
A few practical points that make the ambulance arrival smoother:
- Know the address of the service — the full street address, the suburb, the postcode, and any unit or building number. Have it written by the phone.
- Know the access route — the nearest street, the gate, the door the paramedics should use, whether there is parking.
- Have someone available to meet the ambulance — to wave them in, hold doors open, and direct them to the casualty.
- Clear the path — remove obstacles, move other children away, clear furniture if necessary.
- Have the child accessible — in an open space where paramedics can work, not in a corner of a crowded room.
- Have the documentation ready — enrolment file, medication file, action plan, anything that supports the handover.
These are small things and they can be done in parallel with the call to 000 — usually by a second educator while the first stays with the child. The investment of a few minutes of preparation makes the difference between a smooth handover and a chaotic one.
The first aider's role in serious illness or injury includes prompt recognition, immediate first aid, calling for additional help including emergency medical services where indicated, and providing a clear and complete handover to the next level of care. The handover should include the casualty's identity, the time and mechanism of the incident, the signs and symptoms observed, the first aid that has been given, and any relevant medical history including known conditions and medications. The first aider should remain with the casualty until handover is complete, should provide ongoing first aid as needed, and should support the casualty's family and any others affected by the incident.
What not to do
- Do not delay calling 000 because you are not sure if the situation is serious enough. The dispatcher will help.
- Do not delay calling 000 because you cannot reach the parents. The ambulance is for the child; the parents will catch up.
- Do not treat "call the parent" as the complete response when the child needs more.
- Do not hang up on the 000 dispatcher until they tell you to.
- Do not leave the child unattended while you make calls — get another educator to help, or use a phone in the room.
- Do not give a vague handover. Be structured, be specific, be brief.
- Do not forget to send the child's medical information with the paramedics.
- Do not consider the response complete when the ambulance leaves. Documentation, debrief, family follow-up, and Regulatory Authority notification are all still ahead.
You will rehearse the 000 call on a simulated phone, including the address, the location, the description of the child, the response, and the staying-on-the-line until told to hang up. You will also practise the ATMIST handover to a simulated paramedic and the parent phone call for several different scenarios. The technique is the same as for any high-stakes communication: structure, brevity, accuracy, calm.
The decision to escalate a sick child up the chain of care is the most consequential decision an educator makes in a paediatric emergency. Match the response to the urgency, call the right service, give a clean structured handover, stay with the child until someone else is in charge, and document everything afterwards. The 000 dispatcher is your ally; use them. The parent is the partner; communicate with them. The paramedics are the next link in the chain; brief them well. Most of these calls happen smoothly and most of the children involved go on to recover. Your part is to make sure the chain works at the moment it needs to.
— ANZCOR Guideline 10.1 (principles for the use of first aid)
